Originally published by our sister publication Anesthesiology News
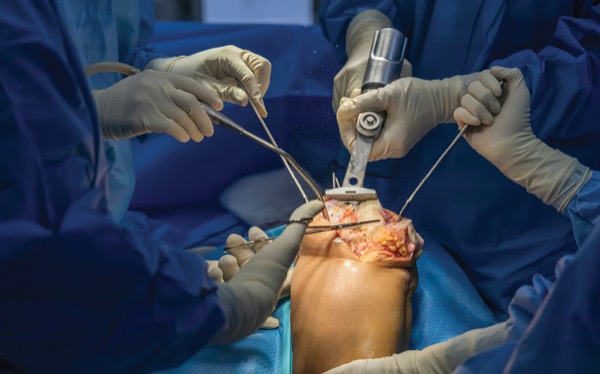
PHILADELPHIA—Same-day outpatient total knee arthroplasties (TKAs) and total hip arthroplasties (THAs) are projected to increase from approximately 15% of all cases in 2016 to 50% by 2026, according to a 2017 study (Curr Rev Musculoskelet Med 2017;10:567-574).
“By 2026, there may be more outpatient than inpatient total joint arthroplasties [TJAs],” said Eric Schwenk, MD, the director of orthopedic anesthesia at