Updated 12/11/23
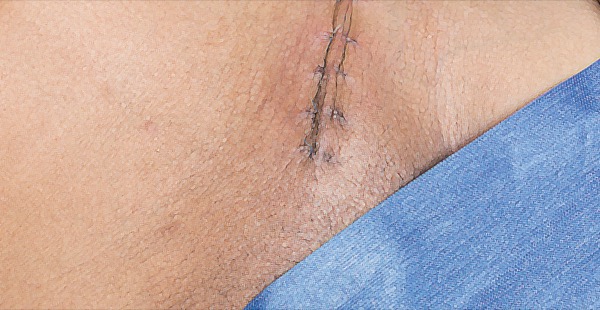
Peripheral nerve stimulation (PNS) can be an effective treatment for neuropathic pain after surgery or trauma to the groin.
While appendectomies and cesarean deliveries can cause sustained pain in the groin, chronic neuropathic groin pain is most commonly associated with herniorrhaphy.
An estimated 13.6% of patients experience chronic groin pain four months after hernia repair surgery. Of those, nearly 40% are diagnosed with neuropathic pain, studies have shown.
Percutaneous