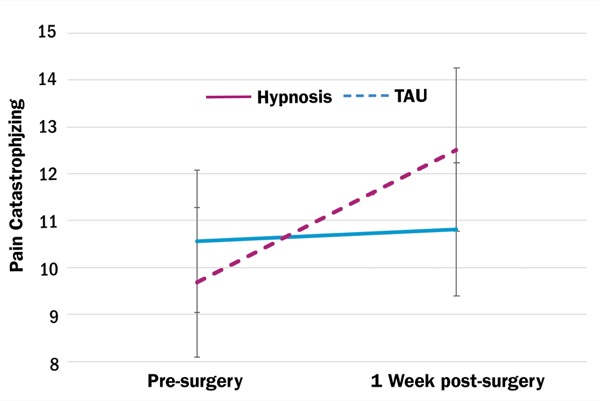
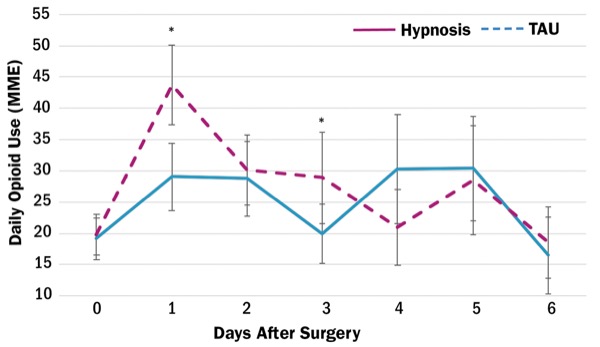
Clinical hypnosis for pain management can help reduce opioid consumption after surgery, according to a study in adults undergoing major oncologic surgery. The study, published in the Journal of Pain Research, suggests that clinical hypnosis may be a viable opioid-sparing adjunct treatment for pain, at least in certain patients.
“There have been studies showing that clinical hypnosis is effective for pain relief in the days after surgery, but little research into how it affects opioid