Originally published by our sister publication Anesthesiology News

Icahn School of Medicine at Mount Sinai
New York City
Hospital for Special Surgery
Department of Anesthesiology
Weill Cornell Medicine
New York City
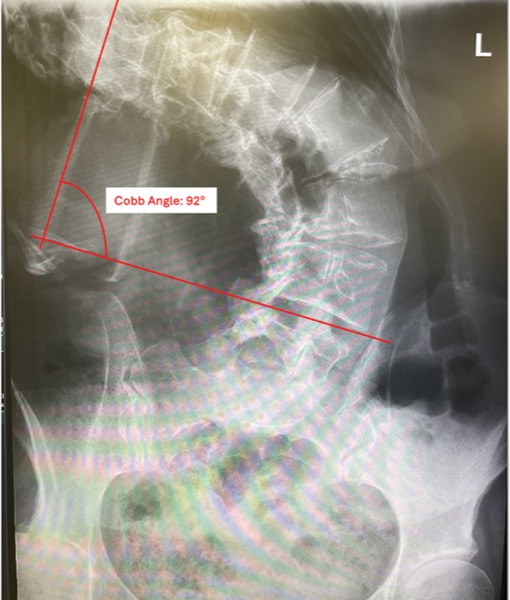
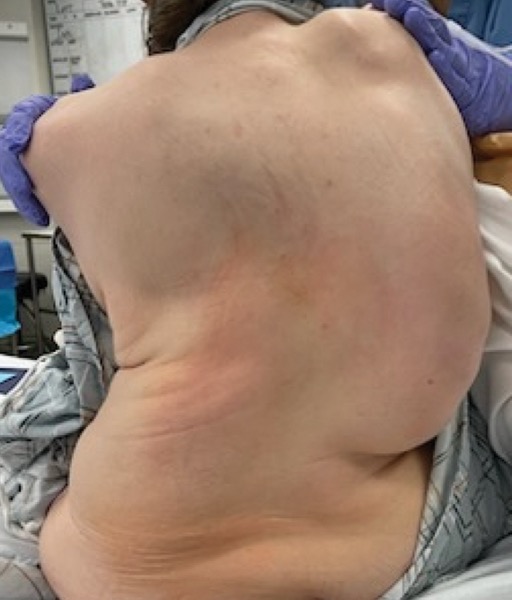
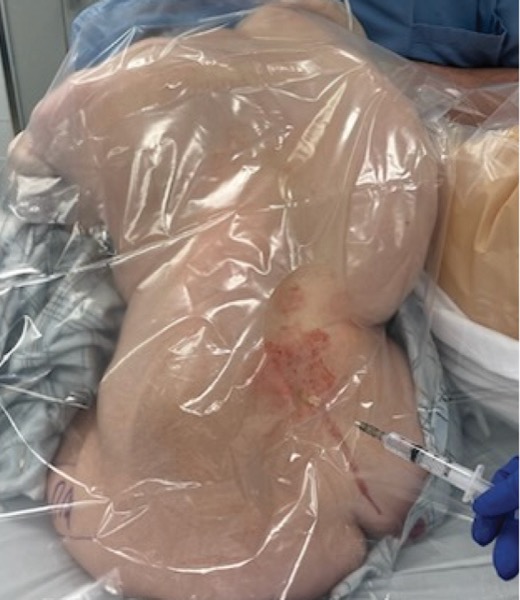
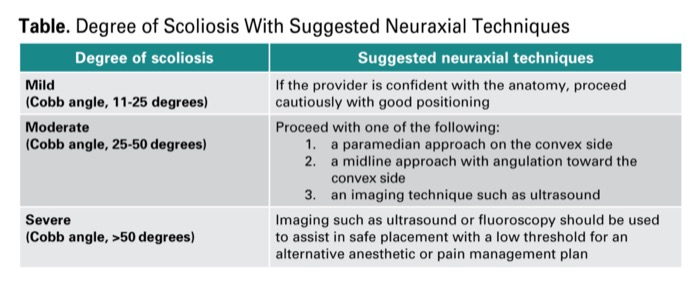
For patients with severe scoliosis, careful preoperative planning is paramount for intraoperative and postoperative care