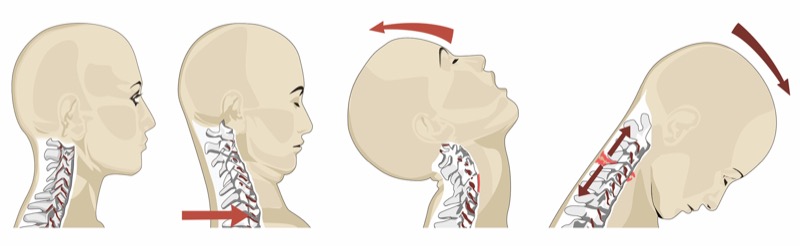
New research suggests within three days of a whiplash injury, clinicians can predict which patients will develop chronic pain based on the extent of “cross talk” between two regions of the brain and the person’s anxiety level after the injury (Nat Ment Health 2024;2:1362-1370).
The study, conducted at the Technion – Israel Institute of Technology, Northwestern University and McGill University, included more than 200 whiplash patients, 177 of whom completed functional MRI