Originally published by our sister publication General Surgery News
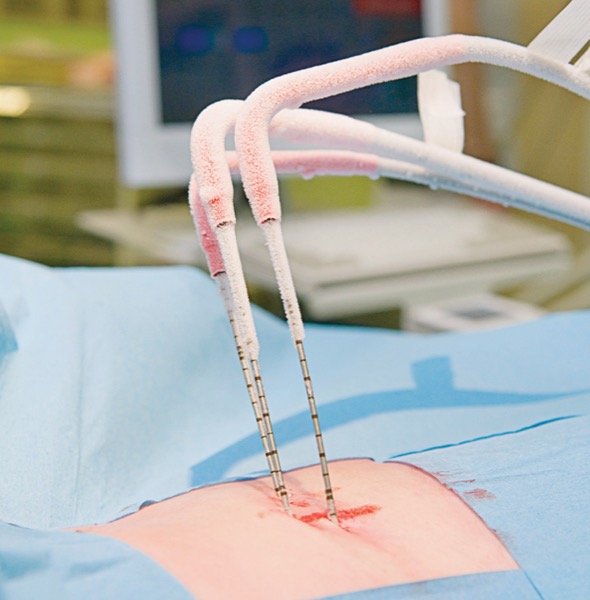
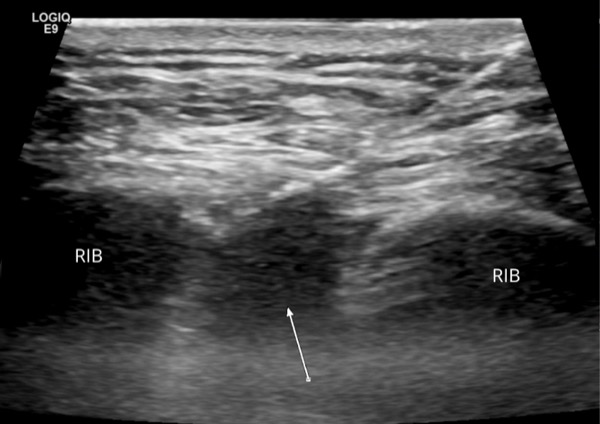
In patients undergoing abdominal wall surgery, cryoablation administered subcutaneously up to a month before surgery is showing potential to keep them numb and free of pain for weeks and possibly months after surgery, reducing or eliminating the need for narcotic painkillers while they recover, according to one institution’s experience.
Ian Hodgdon, MD, an associate professor of surgery at