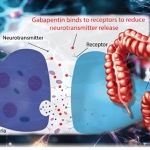
A recently published literature review indicates that there is a lack of data proving the efficacy of opioids versus placebo for relieving persistent cancer pain.
Constant cancer pain is defined as pain that is continuous and relatively constant when a patient is at rest.
“These findings challenge the widely held view that opioids are the most powerful pain relievers for moderate to severe pain,” study researcher Christina Abdel Shaheed, PhD, a National Health and Medical Research