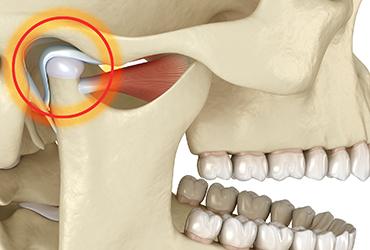
A recently released guideline recommends adult patients with temporomandibular disorder (TMD)-associated chronic pain should consider noninvasive/nonpharmacologic treatments before surgery or drugs.
“Our guideline found evidence that patients should first consider conservative therapies directed at optimizing coping and promoting movement and activity,” guideline author Jason W. Busse, MD, a professor of anesthesia and Michael G. DeGroote National Pain Centre faculty member at